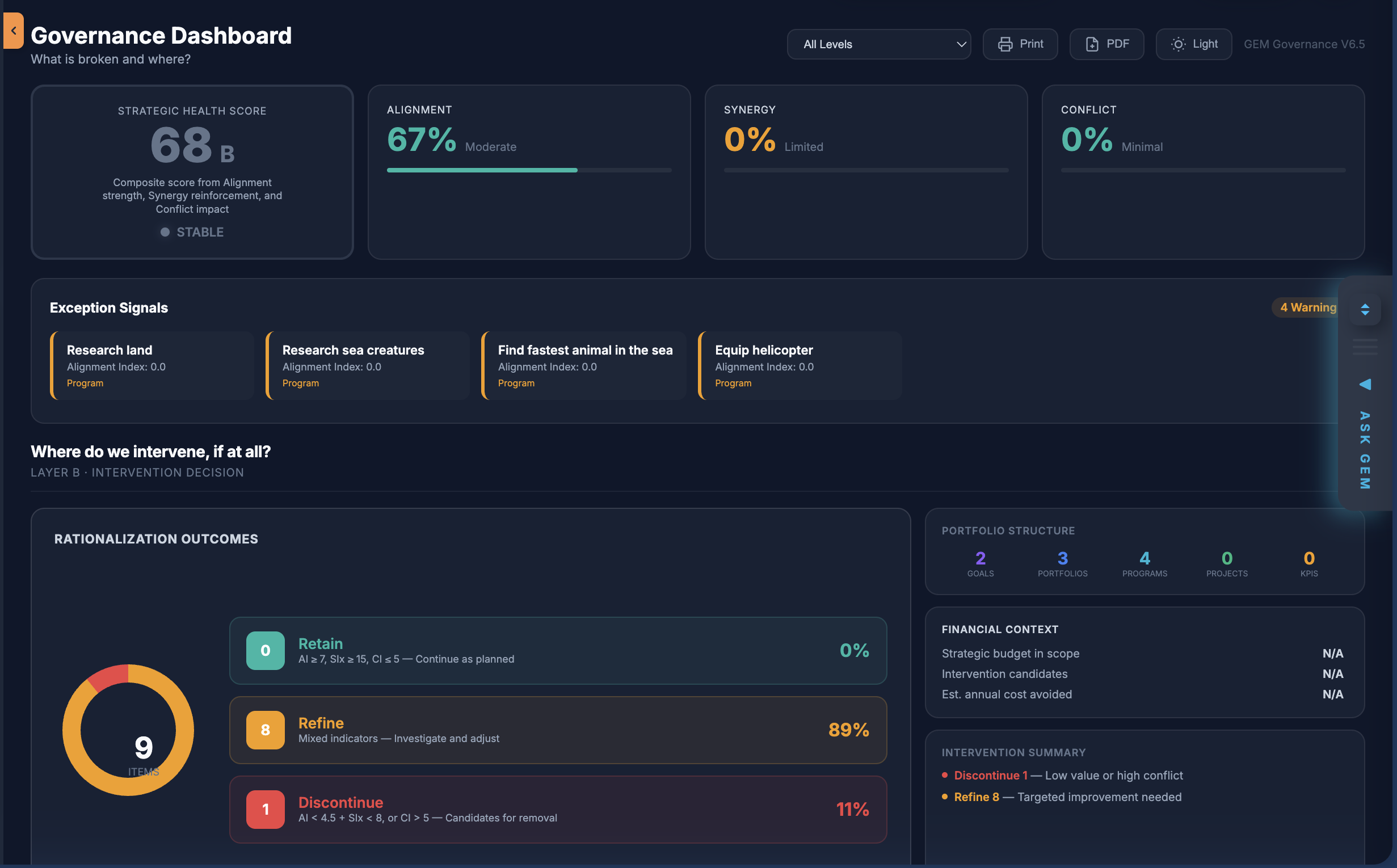
- Enterprise-Wide Strategy Execution Strategy Execution System Setup. Strategy Implementation Governance.
- Regional & Business Unit Strategy Execution Strategy Execution System Setup. Strategy Implementation Governance.
- Department & Functional Strategy Execution Strategy Execution System Setup. Strategy Implementation Governance.
- Strategy Execution Audit Execution system setup review. Governance structure assessment.
- Portfolio Governance Capital allocation discipline and structured portfolio oversight.
- Program Governance & Oversight Executive reporting cadence and cross-functional program coordination.
- Project Management & Governance Structured project delivery and governance discipline aligned to strategic objectives.
- Execution Risk & Dependency Management Identification and mitigation of structural execution fragility.
SAF designs and operates institutional execution architectures, supported by a proprietary execution system that sustains alignment, governance discipline, and execution predictability continuously, not episodically.